

Prices from £18.00
In stock. Simply fill in a brief consultation questionnaire and one of our doctors will review your request today.
-
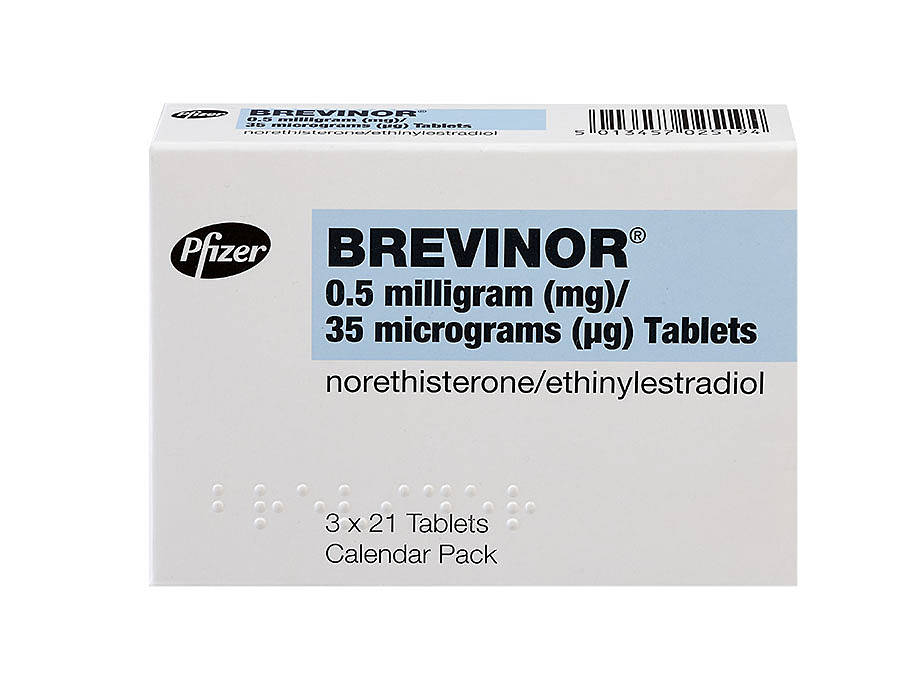
Brevinor is an effective combined oral contraceptive pill, which contains two hormones that work to prevent you from getting pregnant.
After getting your first prescription from your GP or sexual health clinic, you can order repeat prescriptions from our ZAVA Doctors online.
If you're looking for a pill with fewer side effects, Brevinor could be a great choice. As a second-generation combined pill, Brevinor has less oestrogen effects than some other pills.



About Brevinor
-
-
Brevinor is a combined oral contraceptive pill which contains two hormones: oestrogen and progesterone.
Brevinor works by:
- preventing eggs from being released by the ovaries (ovulation)
- making the cervical mucus thicker
- and making the uterus not suitable for a fertilised egg to attach to
When used correctly, Brevinor is around 99% effective at preventing pregnancy.
The active ingredients in Brevinor are 500 micrograms of norethisterone (progestin) and 35 micrograms of ethinyl estradiol (oestrogen).
-
-
Brevinor should be taken 21 days in a row, with a 7-day break period afterwards. Ideally, you should take the Pill at the same time every day. You have to take it within 24 hours of the same time every day.
You should continue with this pattern of taking the pill (21 days on the pill followed by a 7-day break) even if you’re still having your period at the end of the 7-day break.
If you forget to take one pill, take it as soon as you remember and continue the with next pill as normal. You will still be protected from pregnancy.
If you‘ve missed 2 or more pills, or you start taking the pill again late at the end of your 7-day break you should start taking the pill again and also use another form of contraception such as condoms, for the next 7 days to prevent pregnancy. You may also need to take emergency contraception if you have had unprotected sex before missing the pills.
If you’ve had vomiting or diarrhoea while taking the pill, it might not be as effective anymore. If either of these continue for more than 24 hours, you should also use another form of contraception such as a condom for 7 days after you recover.
Always contact your online doctor or GP for advice if you’re unsure about how you are meant to be using the contraceptive pill.
-
-
There are about 23 different combined oral contraceptive pills available in the UK today, and women can react differently to different types of Pill.
The reviews of using Brevinor pills are mixed. Some women say they had little or no side effects, and some have reported mood swings, migraines, and feeling sick.
Some others have also reported that using Brevinor helped to reduce their acne breakouts and migraines.
-
-
There’s no clear evidence that using the pill can cause weight gain. But, the Pill can cause short-term, temporary weight gain because of your body retaining water. This weight gain isn’t permanent, though.
If you are concerned about your weight, you can get advice on weight management from your GP. They can give you advice, like diet changes and increasing your exercise levels.
-
-
Compared to some other Pills, Brevinor has effects that help to control acne. It can also help to reduce heavy and painful periods.
If you do experience acne, or have any concerns about acne in general, you could think about getting acne treatment.
Pills like Yasmin also help with reducing acne and heavy periods. However, Brevinor is relatively cheap compared to Yasmin.
-
-
Brevinor may not be suitable for you if you:
- have irregular periods
- have just given birth
- have health conditions that make Brevinor unsafe
- are taking other medications that make Brevinor unsafe
- smoke or are obese
- are breastfeeding or think you may be pregnant
-
-
To order Brevinor from our online service:
- Fill in a medical questionnaire and answer a few simple questions about your health
- One of our registered doctors will review your order and check if Brevinor is right for you
- You can then choose your delivery option at the checkout which may vary depending on the pack size and dosage you’ve chosen
- Your medication is then posted by our pharmacy, either to your preferred address of a local post office for you to collect from
-
-
While taking Brevinor, you may get the following side effects, especially within the first few weeks:
- Breast pain, enlargement, and tenderness
- Mood changes
- Change in your sex drive (libido)
- Headaches
- Dizziness
- Anxiety
- Pelvic pain
- Stomach upset
- High blood pressure
- Breakthrough bleeding
- Skin reactions
- Chest pain
- Back pain
- Vaginal infections with discharge
- Contact lens irritation

Dr Kathryn Basford is a qualified GP who works as a GP in London, as well as with ZAVA. She graduated from the University of Manchester and completed her GP training through Whipps Cross Hospital in London.
Meet our doctorsLast reviewed: 08 Feb 2019
-
EMC. (2018). Brevinor tablets. [online] Available at: https://www.medicines.org.uk/emc/product/1145/smpc#PRODUCTINFO [accessed 10th December 2018].
-
Netdoctor (2018). Brevinor. [online] Available at: https://www.netdoctor.co.uk/medicines/sexual/a6330/brevinor-ethinylestradiol-and-norethisterone/ [accessed 10th December 2018].
-
Patient.info (2018). Combined hormonal contraceptives. [online] Available at: https://patient.info/medicine/combined-hormonal-contraceptives [accessed 10th December 2018].
Contraceptive pills are a reliable way of reducing your risk of getting pregnant from sex. ZAVA offers most common brands of pill, so you can order your preferred brand by visiting our contraceptive pill service page.
In stock. Prices from £18.00








